Malaysia needs a refreshed strategy on how to accelerate the much-needed digital transformation in the Malaysian healthcare eco-system

On July 25, 1997, Malaysia was one of the first Asian countries to launch a National Telemedicine Blueprint, as a part of the world-famous Vision 2020. This was thought to be a paradigm shift and meant to transform Malaysian healthcare way forward in the future.
After 24 years now, this transformative vision, remains as a vision, with many projects attempted, but failing to materialise. This article is not meant perform an analysis into the implementation of this visionary blueprint, but it will however explain on how to accelerate the much-needed digital transformation in the Malaysian healthcare eco-system.

There are three general phases in any “Digital Transformation” (refer to Figure 1.0).
They are Digitisation, Digitalisation and Digital Transformation.
Digitisation is the first phase of transformation and is described as “the conversion from analogue to digital”. Before any change in process can take place, the data/information/source must be transformed into a digital form. This refers to the conversion of healthcare data, on paper or similar to be transformed into a digital data. This paves the way for the next stage, “Digitalisation”.
Digitalisation relates to “the process of using digital technology to digitalise a process”. It basically means how do we use digital technology and change processes for the better.
In healthcare, this applies to a wide variety of processes, right from patient registration at hospitals to how doctors use AI to diagnose the patient’s condition to how to predict the next Covid-19 cluster or pandemic.
Finally, Digital Transformation transforms the business of the healthcare organization beyond the scope of a particular process or department. Digital Transformation opens the organization to a blue ocean of business possibilities, enabling new ways of doing things, disrupting the industry, delivering new value to patients and partners.
Instead of patients going to the hospitals, the physicians are now able to speak, diagnose and prescribe medication through video conference, while patients are at home, hence increasing the market share, even during the pandemic.
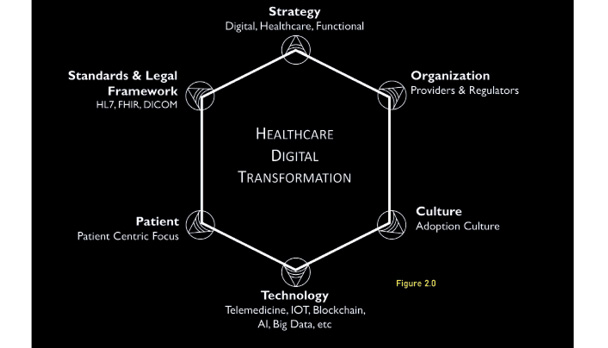
In Malaysia, we had some progress in Digitisation and Digitalisation in silos, but the overall digital transformation leaves much to be desired. In order to accelerate the overall transformation, six key areas need to be focused on (refer to Figure 2.0).
Strategy & Implementation:
While the 1997 blueprint was a good strategy document, it translated to poor implementation. Malaysia now needs a refreshed strategy, from the government sector which encompasses the overall healthcare landscape, for an inclusive healthcare eco-system, which provides a platform for public and private provider, payor, physicians, patients and partners.
This will enable the usage of digital technology to lower cost, while providing a higher quality of care for patients. This is the first step to accelerate the digital transformation and as such, each sector in the industry needs to know their role to translate strategy into action.
Organisation structure
Malaysian healthcare organisations must embrace an internal collaborative approach to achieve digital transformation. Todate, one of the stumbling blocks of a paradigm shift within Malaysian hospitals and healthcare organisations are internal users.
The physicians need to work closely with patients. The hospital operations team needs to understand clearly the KPI which is being measured for the transformation and appreciate and adopt the technological changes that are being brought into the picture.
All this collaboration requires a digital transformation champion to drive it through, with the senior management’s endorsement. The stakeholders need to understand that digital transformation requires real investment of time, budget, manpower allocation, training, knowledge sharing and most importantly, political will.
And finally, to accelerate digital transformation, the organisation needs to be agile and be ready for change. The hardest part of the digital transformation is the constant change which it brings.
Hence, an organisation needs to be able to respond quickly to changes in healthcare technology and market environment by moving away from traditional hierarchies and embrace leaner and flatter organisational structures.
This is especially true in the current VUCA (volatile, uncertain, complex and ambiguous) state of the world.
Culture
Healthcare culture must be approached from multiple angles to accelerate the digital transformation. Without the cultural change, the paradigm shift which digital transformation brings will not be sustainable.
The digital transformation requires freedom to experiment, room for creativity and fast adoption & corrective. This is often referred as a “fail forward culture”, meaning that the culture allows to experiment and to learn from mistakes.
Australia’s PCEHR (Personally Controlled Electronic Health Record), launched in 2012, while it had many issues in its early days, was quickly revived and now proves to be a jewel of the Australian’s government strategy for its Covid-19 management.
From changing the patient opt-in to opt-out model, to publishing new integration methods, the Australian government’s Digital Health Agency embraced the “fail forward culture” resulting in the adoption of its National Healthcare Digitalisation, now known as “My Health Record”.
Patient
As the saying goes, “take care of the patient, and the rest will fall in place”. Digital Transformation in any industry focuses on the end customer, and in healthcare, the patient is the customer.
It should be the goal of Healthcare Digital Transformation to empower the patient by enabling interactions between patients, healthcare professionals and other stakeholders and make patients aware of their health conditions and treatment possibilities.
This leads to engagement, coordination, and cooperation with patients – providing more data through their PHR (Patient Health Record) system, in and out of hospitals, hence increasing digitisation and digitalisation, leading to overall faster digital transformation through EMR and eventually, EHR.
Standards and Legal Framework
A national level standard which is driven by regulators is required for hospitals to share data, for patients to use remote patient data monitoring devices and to enable national e-prescription infrastructure, PHR, EMR and EHR. Old standards like HL7 and DICOM, paired with new ones like FHIR has to be adopted, endorsed, mandated, and enforced in our Digitisation and Digitalisation effort.
Once the standards are in place, digital transformation can be accelerated with workshops to motivate all industry players on the importance of the standards. Another important aspect would be the legal framework to protect the patient’s data, physicians telemedicine practice, hospital’s digital workflow and overall industry security from data and operations point of view, failing which, the digital transformation will not be sustainable.
Technology
This is the last but the most important piece of the Digital Transformation, the Technology. While healthcare organisations can get carried away with rolling out technologies, it is important to keep the balance by using the “Functional Strategy” to map the “Digital Verticals” in the Digital Strategy to the Healthcare Strategy.
The technology which enables digital transformation is limitless, but it has to be guided by the healthcare and functional strategy. Malaysia launched one of the world’s first National Telemedicine Blueprint but now it is lagging its neighbouring countries.
By 2050, it is expected that 20 per cent of Malaysian will be aged 65 years and above, making us a “super-aged” society. The benefit of digital healthcare is immense and now is the time to accelerate Healthcare Digital Transformation. — The Health
G Saravanan is a Director of Consulting at Ainqa Health Sdn Bhd.








